I’ve previously written about the benefits of squatting for ailments of the gastrointestinal tract, specifically diverticulitis and hemorrhoids. Some argue that squatting to defecate can prevent all manner of illness and while there are some clinical conditions I’d like to explore further in the squatting-in-the-bathroom paradigm, today I want to write about something quite different.
I finished my Obstetrics and Gynecology clerkship 5 weeks ago. I did my clerkship at a large, and rather posh, private hospital that is affiliated with my medical school. There are some great doctors there, but I was sometimes aghast at the rather aggressive approach to delivery that many took. The cesarean section rate for the last year was 47%, well above the national average of 33%, and most labors were artificially augmented. I did not witness a single VBAC (Vaginal Birth After Cesarean), and was told that only one of the house attendings would perform them.
On the first day of my clerkship, I asked the clerkship director if women delivered in a variety of positions or if they were restricted to delivering in lithotomy (what many today think of as the “traditional” birthing position with the mother on her back with her feet in stirrups). The director seems to be a rather progressive woman (she is the driving force pushing the hospital to become a “baby-friendly hospital”) and she gave me a rather knowing look and said “I know what you’re getting at, but unfortunately everyone here delivers lying down”.
Indeed, as I went through my rotation, all the vaginal deliveries I saw were done in the semi-reclined position that is common in western hospitals. This is not universally true. When I ask my family physician (who actually delivers babies- quite a rarity in this day and age) what position her patients delivered in, she immediately responded “whatever position they’re most comfortable in!”, a response I have heard from a few other MDs as well as many midwives and labor coaches.
Birth is, of course, a risky thing… Death in childbirth was historically a significant cause of mortality, and the rates are still high in some countries. I think it’s important to recognize that birth is still a risky endeavor, and while pregnancy and labor is a normal human experience, it is one that comes with real dangers. Nonetheless, just because historic rates of maternal demise were much higher than they are today does not mean we should not cast an eye to historic practices when thinking about birth. As I’ve argued before, I think modern medicine (in obstetrics and in most fields) could greatly benefit from casting an eye to evolution and our ancestors to further improve our current medical system by combining ancestral and evolutionary knowledge with modern technology and science.
I planned to write a significant argument for the consideration of “non-traditional” (though they are, in fact, traditional) positions for laboring, but then I came across a book from 1883 that said it all already. The book, entitled Labor Among Primitive Peoples (with the subtitle Showing the development of the obstetric science of today from the natural and instinctive customs of all races, civilized and savage, past and present.) by George Julius Engelmann MD, is available in it’s entirety thanks to the power of Google Books.
This book is fascinating, and at many times frightening (more on that later), but I found the “Posture in Labor” chapter of particular interest for this post. There, the author divides the positions into 3 main categories: Perpendicular (including standing, partially suspended, and suspended), Inclined (including sitting erect, squatting “as in defecation”, kneeling, and semi-recumbent), and horizontal (on the back, side, or chest and stomach (!)). He also goes through the then common birthing practices of countries in Europe, Asia, Africa, North America, Central and South America, and Australia and the surrounding islands [1].
Curious?- here are some highlights from the book, but I highly recommend you take a scroll through the book to at least see the illustrations!

The squatting position of the Tonkowas- a Native American group indigenous to present-day Oklahoma and Texas.

The squatting tradition of the Pawnee Native Americans- the laboring mother squats with her back to a female assistant while someone (in this case a shaman) assists with the delivery. This position (with an assistant acting as a back support) was apparently popular in many cultures around the world.
There is plenty to be said on each of the positions mentioned, but for the sake of this post I will focus on what the author says on squatting. He states that squatting
is hardly to be defined with exactness, yet we may, in a general way, consider all postures as squatting which resemble that assumed in defecation. Though apparently inconvenient, and repugnant to the refined woman, this position is certainly the most natural one for expulsion from the abdominal or pelvic viscera, and will certainly, in many cases, facilitate labor. (72)
He documents the experience of another physicians, saying:
“… he tells me of attending a lady of good position in society in two labors. ‘In her first labor, delivery was retarded without apparent cause. There was nothing like impaction, or inertia, yet the head did not advance. At every pain she made violent efforts, and would bring her chest forward. I had determined to use the forceps, but just then, in one of the violent pains, she raised herself up in bed and assumed a squatting position, when the most magic effect was produced. It seemed to aid in completing delivery in the most remarkable manner, as the head advanced rapidly, and she soon expelled the child by what appeared to be one prolonged attack of pain. In subsequent parturition, labor appeared extremely painful and retarded in the same manner; I allowed her to take the same position as I had remembered her former labor, and she was delivered at once squatting.” (73)
Information on traditional birthing positions can also be wrought from the Old Testament. The King James translation of Exodus 1-16 says “When ye do the office of a midwife to the Hebrew women, and see them upon the stools…”. However there is some scholarly debate about the translation of the word “stools”, as a more accurate translation might actually be “stones”. You might wonder what stones have to do with birthing, until you see this depiction of a popular Persian birthing position.
A friend recently shared a video of women delivering in the squatting position. I post this video with the STRONGEST OF WARNINGS. I warn (only slightly jokingly) that that which is seen, cannot be unseen*. Proceed at your own risk! Birth is magical (though not mysterious), but some people find the imagery rather disturbing.
With that warning in place, I present the following video:
Those that have seen (or perhaps experienced) birth in the modern conventional position will probably agree that these women make labor look somewhat easy…
It’s also interesting to explore the delivery position of some of our closest living ancestors. It appears that chimpanzees naturally deliver in a squatting position (with a similar “occiput anterior” presentation).
One of the most basic elements of obstetrics that we learn in medical school is the “7 cardinal movements” of delivery. Medical student must know these movements- engagement, descent, flexion, rotation, external rotation, and expulsion- and on the labor and delivery floors we are expected to participate in and assist with deliveries. I remember watching many of my classmates “air-deliver” babies- going through the maneuvers of “catching” (a much more honest term than “delivering”) a baby, as we discussed these cardinal movements. While I understand that it is important to know these normal movements, the idea that a physician actually guides these movements is laughable. Truly, in most deliveries, our hands are there to catch and support. In fact, they are likely only necessary because of the position that we have developed for women to deliver. In this youtube video explaining the 7 cardinal movements, the doctors hands only show up once the head is expulsed so that the baby’s head does not rest on the perineum. Indeed, “protect the perineum” is the mantra chanted to med students and novice doctors learning to deliver babies in a reclining position. In the squatting position, gravity protects the perineum.
Gravity isn’t the only reason to consider delivering in a squatting position. I’ve heard it said (though haven’t found a reliable source) that squatting not only increases a woman’s ability to push (allowing her to better utilize her abdominal muscles), but also helps the pelvis open wider for delivery (due to the pull of abducting muscles). In this position, and with the aid of gravity, it seems (and again I’ve heard it suggested) there is a lower risk of a perineal tear, something that I saw all too frequently during my Ob clerkship.
Squatting is by no means a perfect solution to birthing. According to at least one study conducted in Nepal, squatting deliveries (along with multiparity and early age of first birth) are associated with an increased risk of pelvic organ prolapse later in life [2]. Also, opting for a squatting delivery removes the option of an epidural for pain control. An epidural causes a loss of sensation below the level of anesthesia, thus making walking (and squatting) impossible.
Squatting is not the only traditional (though now it would be classified as “non-traditional”) birthing position that women can consider. I whole-heartedly appreciate my family physician who encourages women to find a position that is most-comfortable for them. Hands-and-knees (exactly what it sounds like), has actually been studied in the first stage of labors for mothers whose babies are delivering in the occiput-posterior position. While the study was small, the findings were encouraging [3].
Sometimes when I talk about evolutionary and ancestral medicine people assume that I am anti-modern medicine. I am not. In childbirth in particular, modern advances in general health, pre-natal care, diagnostics, medicine, and surgery have saved countless lives. I am, however, in favor of assessing (and re-assessing) our beliefs (new and old) about how to best obtain and preserve health.
I find Dr. Engelmann’s book fascinating, and while there are elements that are rather disconcerting (the traditions of male and female circumcision, a surgery performed on men to decrease fertility, and the tradition in one culture of removing one testicle to prevent the conception of twins to name a few), I find his observations and his humble admissions (as well as his love of commas) lovely. His conclusions are well worth reading (emphasis mine):
Abler obstetricians than myself have undoubtedly understood the movements of women, and the positions which they assumed in the agony of the expulsive pains. As regards myself, I must candidly confess this was not the case; and it was not until I had undertaken this work, and had begun to study the positions assumed by savage and civilized people during labor, that I began to understand that there was a method in the instinctive movements of women in the last stage of labor. I had seen them toss about and sought to quiet them; I bade them have patience and lie still upon their backs; but, since entering upon this study, I have learned to look upon their movements in a very different light. I have watched them with interest and profit, and believe that I have learned to understand them. It has often appeared to me, as I sat watching a tedious labor case, how unnatural was the ordinary obstetric position for the parturient woman; the child is forced, I may say, upwards through the pelvic canal in the face of gravity, which acts in the intervals between the pains, and permits the presenting part of the child to sink back again, down the inclined canal. If we look upon the structure of the pelvis, more especially the direction of the pelvic canal and its axis, if we take into consideration the assistance which may be rendered by gravity, and, above all, by the abdominal muscles, the present obstetric position seems indeed a peculiar one.
The contractions of the previously inactive and rested abdominal muscles are a powerful adjunct to the tired uterine fibre, in the last prolonged and decisive expulsory effort, and in the dorsal decubitus they are somewhat hampered; they act to the best advantage in the inclined positions, semi-recumbent, kneeling, or squatting. We know that the squatting position is the one naturally assumed if an effort is required to expel the contents of the pelvic viscera; we, moreover, all know how difficult, even impossible, it is for many to perform those functions recumbent in bed, and mainly because they have-not sufficient control of the abdominal muscles in that position. Much more is this the case in the expulsion of the child; but the recumbent position is sanctioned by custom; it is pointed out as apparently convenient; it is imperatively demanded by prudery; and by a false modesty which hides from view the patient’s body beneath the bed clothes; and above all it is dictated by modern laws of obstetrics, the justice of which I have never dared question; we have all been taught their correctness, and we all thoughtlessly follow their dictates. There is no reason for assuming this position, though we are taught it; it is not reason, or obstetric science, but obstetric fashion which guides us,- guides us through our patients; and blindly do we, like all fashion’s votaries, follow in the wake. (140-141)
Obstetrics is a specialty where many do not want to question the norm. Indeed, fear of litigation generally pushes physicians to be overly aggressive in managing labor and quick to opt for cesarean delivery. Randomized controlled studies that push the boundaries of modern “obstetric fashion” are unlikely to be performed for fear of litigation, but observation of mothers who choose to deliver in various positions as well as consideration of ancestral practices can potentially help drive modern medicine to a higher standard.
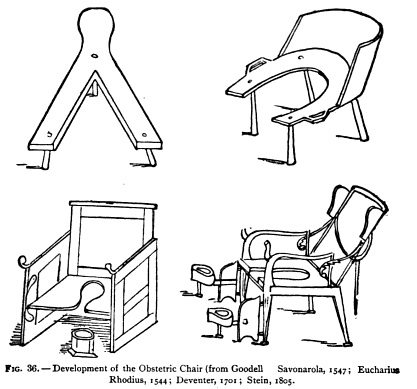
The “progression” of the obstetrical chair. The first stool is not unlike some modern birthing stools, while the final incarnation is not too far displaced from the modern delivery-room bed.
*A brief story from when I was on an Emergency Medical Services elective. The ambulance I was on was called to back up another team that had gone to attend at precipitous delivery. When we arrived, it became apparent that we were not there to assist the patient (it was her fourteenth (!!!) delivery), but rather to make sure that the EMT who had just witnessed his first delivery did not pass out. He had a very pale and shocked look to him, and he just stared at us blankly as we helped the mother with her new child. After a couple minutes, he looked at us and asked “does the mental image ever go away?”. He later admitted that he didn’t want to sleep with his girlfriend for at least two weeks… I believe this is what a good male friend of mine describes as figuring out the difference between “medical vagina and sexy vagina”.
1. Engelmann, G.J., Labor Among Primitive Peoples. Second ed. 1883, St Louis: J.H. Chambers and Co.
2. Lien, Y.S., G.D. Chen, and S.C. Ng, Prevalence of and risk factors for pelvic organ prolapse and lower urinary tract symptoms among women in rural Nepal. Int J Gynaecol Obstet, 2012. 119(2): p. 185-8.
3. Stremler, R., E. Hodnett, P. Petryshen, B. Stevens, J. Weston, and A.R. Willan, Randomized controlled trial of hands-and-knees positioning for occipitoposterior position in labor. Birth, 2005. 32(4): p. 243-51.
And finally, for your viewing pleasure, this classic:
















